Impact of Mental Illness on Individuals and Families
The COVID-19 pandemic and the resulting economic recession have negatively affected many people'southward mental health and created new barriers for people already suffering from mental disease and substance use disorders. During the pandemic, about 4 in x adults in the U.South. accept reported symptoms of anxiety or depressive disorder, a share that has been largely consistent, upwards from one in ten adults who reported these symptoms from January to June 2019 (Figure 1). A KFF Health Tracking Poll from July 2020 also found that many adults are reporting specific negative impacts on their mental wellness and well-beingness, such equally difficulty sleeping (36%) or eating (32%), increases in booze consumption or substance use (12%), and worsening chronic conditions (12%), due to worry and stress over the coronavirus. As the pandemic wears on, ongoing and necessary public health measures expose many people to experiencing situations linked to poor mental health outcomes, such equally isolation and job loss.
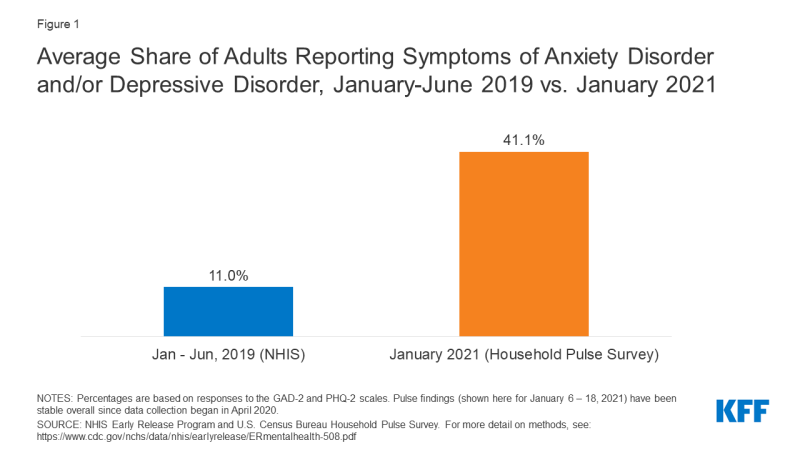
Figure 1: Boilerplate Share of Adults Reporting Symptoms of Feet Disorder and/or Depressive Disorder, January-June 2019 vs. January 2021
This brief explores mental health and substance use during, and prior to, the COVID-nineteen pandemic. Information technology focuses on populations that were particularly at hazard for experiencing negative mental health or substance abuse consequences during the pandemic, including young adults, people experiencing task loss, parents and children, communities of color, and essential workers. Nosotros draw on KFF analysis of data from the Census Agency's Household Pulse Survey (an ongoing survey created to capture data on health and economical impacts of the pandemic), KFF Health Tracking Poll data, and data on mental health prior to the COVID-19 pandemic. Key takeaways include:
- Immature adults have experienced a number of pandemic-related consequences, such as closures of universities and loss of income, that may contribute to poor mental health. During the pandemic, a larger than boilerplate share of young adults (ages 18-24) report symptoms of anxiety and/or depressive disorder (56%). Compared to all adults, young adults are more than likely to study substance employ (25% vs. 13%) and suicidal thoughts (26% vs. 11%). Prior to the pandemic, immature adults were already at loftier take chances of poor mental wellness and substance use disorder, though many did non receive treatment.
- Research from prior economical downturns shows that job loss is associated with increased depression, anxiety, distress, and depression self-esteem and may lead to college rates of substance employ disorder and suicide. During the pandemic, adults in households with task loss or lower incomes report college rates of symptoms of mental illness than those without job or income loss (53% vs. 32%).
- Research during the pandemic points to concerns around poor mental health and well-being for children and their parents, peculiarly mothers, every bit many are experiencing challenges with school closures and lack of childcare. Women with children are more likely to report symptoms of feet and/or depressive disorder than men with children (49% vs. forty%). In full general, both prior to, and during, the pandemic, women accept reported college rates of feet and depression compared to men.
- The pandemic has disproportionately afflicted the wellness of communities of color. Non-Hispanic Black adults (48%) and Hispanic or Latino adults (46%) are more than likely to report symptoms of anxiety and/or depressive disorder than Non-Hispanic White adults (41%). Historically, these communities of color take faced challenges accessing mental wellness intendance.
- Many essential workers continue to face a number of challenges, including greater risk of contracting the coronavirus than other workers. Compared to nonessential workers, essential workers are more likely to report symptoms of feet or depressive disorder (42% vs. 30%), starting or increasing substance use (25% vs. 11%), and suicidal thoughts (22% vs. viii%) during the pandemic.
Both those newly experiencing mental health or substance abuse disorders and those already diagnosed earlier the pandemic may require mental health and substance employ services but could confront additional barriers because of the pandemic.
Prevalence of Mental Illness and Substance Apply Disorder During the Pandemic
During the COVID-19 pandemic, concerns about mental health and substance utilise have grown, including concerns about suicidal ideation. In January 2021, 41% of adults reported symptoms of anxiety and/or depressive disorder (Figure 2), a share that has been largely stable since spring 2020. In a survey from June 2020, 13% of adults reported new or increased substance use due to coronavirus-related stress, and 11% of adults reported thoughts of suicide in the past 30 days. Suicide rates have long been on the rise and may worsen due to the pandemic. Early 2020 data show that drug overdose deaths were specially pronounced from March to May 2020, congruent with the beginning of pandemic-related lockdowns.
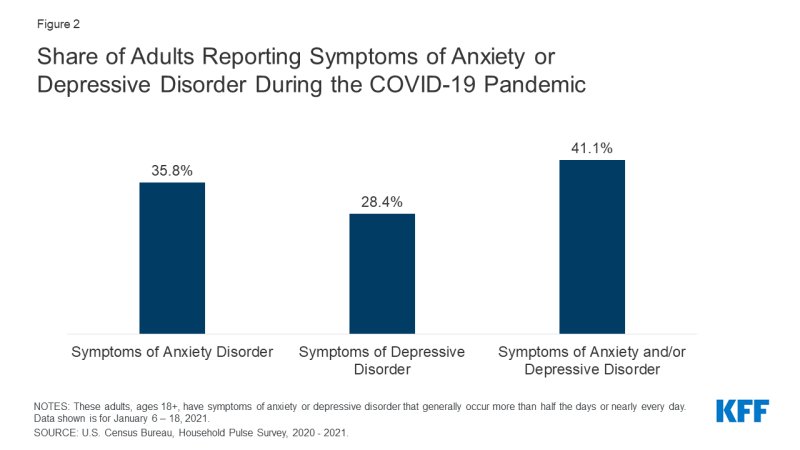
Figure two: Share of Adults Reporting Symptoms of Anxiety or Depressive Disorder During the COVID-19 Pandemic
As was the case prior to the pandemic, adults in poor general health (which may reflect both physical and mental wellness) proceed to written report higher rates of anxiety and/or depression than adults in good general health.1 , 2 For people with chronic illness in particular, the already high likelihood of having a concurrent mental health disorder may be exacerbated by their vulnerability to severe illness from COVID-19. Recently, a written report likewise found that 18% of individuals (including people with and without a past psychiatric diagnosis) who received a COVID-19 diagnosis were subsequently diagnosed with a mental health disorder, such as anxiety or mood disorders. Older adults are also more vulnerable to severe illness from coronavirus and have experienced increased levels of anxiety and low during the pandemic.
Mental distress during the pandemic is occurring against a backdrop of high rates of mental illness and substance use that existed prior to the electric current crunch. Prior to the pandemic, one in ten adults reported symptoms of anxiety and/or depressive disorder. Most one in 5 U.S. adults (47 million) reported having any mental affliction. In 2018, over 48,000 Americans died past suicide,three and on average beyond 2017 and 2018, nearly 11 one thousand thousand adults reported having serious thoughts of suicide in the past year. Additionally, deaths due to drug overdose were four times higher in 2018 than in 1999, driven by the opioid crisis.
There are a variety of ways the pandemic has probable affected mental health, particularly with widespread social isolation resulting from necessary rubber measures. A wide torso of research links social isolation and loneliness to both poor mental and physical health. The widespread feel of loneliness became a public wellness business concern even before the pandemic, given its association with reduced lifespan and greater risk of both mental and physical illnesses. A KFF Health Tracking Poll conducted in belatedly March 2020, shortly after many stay-at-home orders were issued, found those sheltering-in-place were more likely to study negative mental health effects resulting from worry or stress related to coronavirus compared to those not sheltering-in-place.
Some prior epidemics have induced full general stress and led to new mental health and substance use issues. Equally the COVID-19 pandemic continues, different populations are at increased chance to experience poor mental health and may face challenges accessing needed intendance.
Young Adults
Throughout the pandemic, anxiety, low, slumber disruptions, and thoughts of suicide have increased for many young adults. They take also experienced a number of pandemic-related consequences – such as closures of universities, transitioning to remote work, and loss of income or employment – that may contribute to poor mental health. KFF analysis of the Household Pulse Survey finds that throughout the pandemic, a large share of young adults (ages eighteen-24) accept reported symptoms of anxiety and/or depressive disorder – 56% as of Dec 2020 – compared to older adults (Effigy 3).
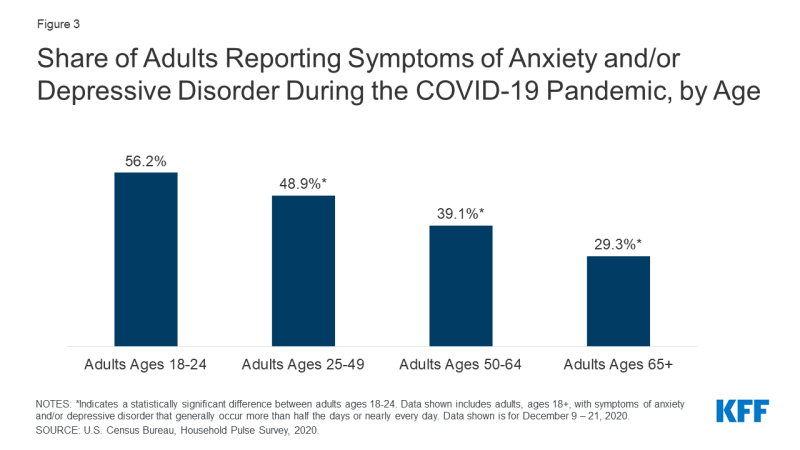
Figure three: Share of Adults Reporting Symptoms of Anxiety and/or Depressive Disorder During the COVID-19 Pandemic, by Age
An earlier survey from June 2020 showed similar findings for young adults relative to all adults. The survey also establish that substance employ and suicidal ideation are particularly pronounced for young adults, with 25% reporting they started or increased substance utilise during the pandemic (compared to 13% of all adults), and 26% reporting serious thoughts of suicide (compared to 11% of all adults). Prior to the coronavirus outbreak, young adults were already at high take a chance of poor mental health and substance use disorder, yet many did not receive handling.
Adults Experiencing Job Loss or Income Insecurity
Throughout the pandemic, many people across the country take experienced job or income loss, which has generally affected their mental wellness. Adults experiencing household job loss during the pandemic have consistently reported higher rates of symptoms of anxiety and/or depressive disorder compared to adults not experiencing household chore loss (53% vs. 32%, respectively; Figure iv). Similarly, findings from the December KFF Health Tracking Poll show that households experiencing income or job loss are significantly more than likely to study that worry or stress over the coronavirus outbreak has negatively impacted their mental health.
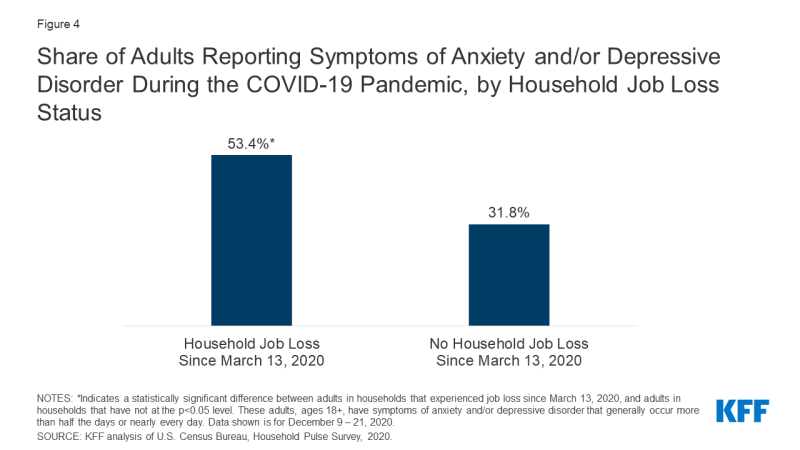
Figure 4: Share of Adults Reporting Symptoms of Anxiety and/or Depressive Disorder During the COVID-19 Pandemic, by Household Job Loss Status
In addition to increased anxiety and depression, job loss may lead to other adverse mental health outcomes, such as substance employ disorder. During the previous recession, the loftier unemployment rate was likewise associated with increases in suicides. A KFF Health Tracking Poll conducted in mid-July 2020 found that, compared to households with no lost income or employment, a higher share of households experiencing income or job loss reported that pandemic-related worry or stress caused them to feel at least one adverse upshot on their mental health and well-being, such as difficulty sleeping or eating, increases in alcohol consumption or substance apply, and worsening chronic conditions (46% vs. 59%, respectively).four
KFF Health Tracking Polls conducted during the pandemic have also establish that people with lower incomes are generally more likely to written report major negative mental wellness impacts from worry or stress over the coronavirus. In December 2020, 35% of those earning less than $twoscore,000 reported experiencing a major negative mental wellness impact, compared to 21% of those with incomes between $40,000 to $89,999 and 17% of those making $xc,000 or more (Figure 5).
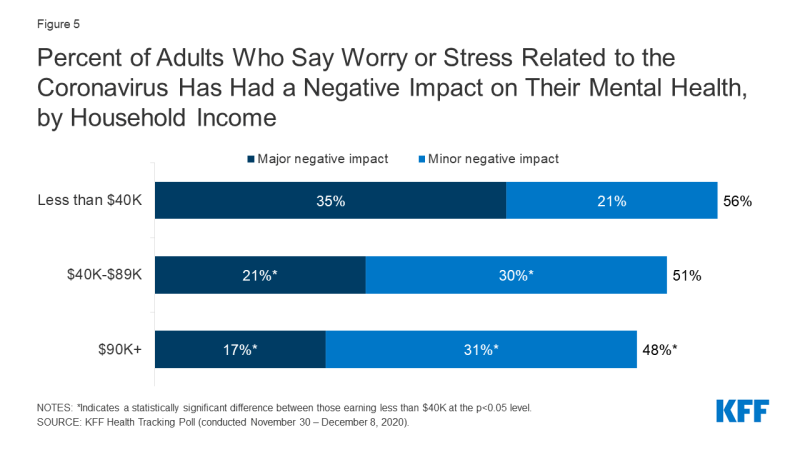
Figure 5: Percent of Adults Who Say Worry or Stress Related to the Coronavirus Has Had a Negative Impact on Their Mental Wellness, by Household Income
Parents and Children
To help deadening the spread of coronavirus, many schools and childcare centers beyond the U.S. have closed and transitioned to virtual instruction for at least some time. With these closures, children and their parents are experiencing ongoing disruption and changes to their daily routines. Research during the pandemic highlights concerns effectually poor mental health and well-being for children and their parents. For instance, many parents with schoolhouse-aged children are now more than concerned about their children's emotional well-being than prior to the pandemic. Both parents and their children accept experienced worsening mental health since the first of the pandemic, and women with children are more likely than their male counterparts to report worsening mental health.
Throughout the pandemic, we notice that adults in households with children under the historic period of 18, compared to adults in households without, are slightly more likely to report symptoms of anxiety and/or depressive disorder (45% vs. 41%, respectively, as of December 2020).v Specifically, amongst households with children under the age of 18, women take been more likely than men to report symptoms of anxiety and/or depressive disorder throughout the pandemic (every bit of Dec 2020, 49% vs. xl%, respectively; Figure 6). Similarly, KFF Wellness Tracking Polls conducted during the pandemic have generally found that amidst parents, women are more probable than men to written report negative mental wellness impacts.half dozen
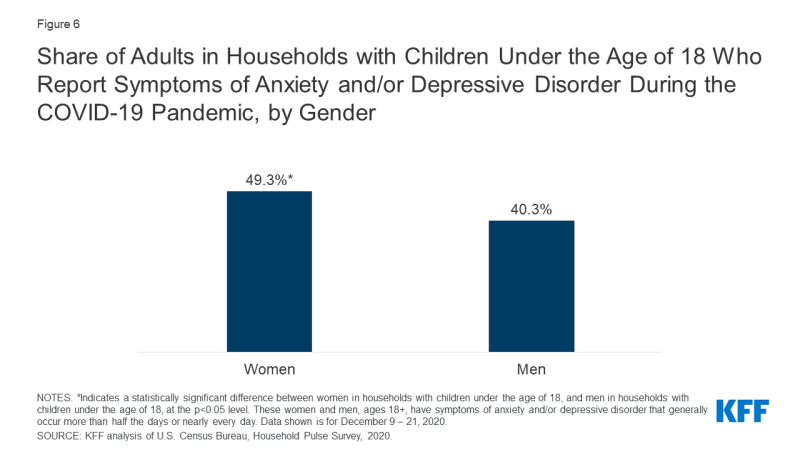
Figure 6: Share of Adults in Households with Children Under the Age of 18 Who Report Symptoms of Anxiety and/or Depressive Disorder During the COVID-nineteen Pandemic, by Gender
Throughout the pandemic, women have been more probable to written report poor mental health compared to men. For example, 47% of women reported symptoms of anxiety and/or depressive disorder compared to 38% of men in December 2020. Amidst women in the workplace, more than one in four are considering leaving their jobs or reducing their hours, with many citing burnout and household responsibilities as the primary reason. Even before the pandemic, women were more than likely than men to report mental health disorders, including serious mental illness.
Existing mental affliction amongst adolescents may be exacerbated by the pandemic, and with many school closures, they do not take the same access to primal mental health services. Prior to the pandemic, more one in ten (16%) adolescents ages 12 to 17 had feet and/or depression.seven Children may experience mental distress during the pandemic due to disruption in routines, loss of social contact, or stress in the household. Additionally, child corruption may be increasing during the pandemic. Kid abuse-related emergency section (ED) visits dropped during the COVID-19 outbreak; however, the severity of injuries among child corruption-related ED visits has increased and resulted in more hospitalizations. Kid corruption tin lead to immediate emotional and psychological problems and is as well an adverse childhood experience (ACE) linked to possible mental illness and substance misuse later in life. Educators play a critical role in the identification and reporting of child corruption. Nevertheless, with school closures and stay-at-dwelling orders, it is likely that many cases are going undetected, and that at-risk children have increased exposure at home to their abusers.
Substance use is also a concern among adolescents. Prior to the pandemic, fifteen% of high school students reported using an illicit drug, and 14% reported misusing prescription opioids. Solitary substance use (as opposed to social use) has increased among adolescents during the pandemic, which is associated with poorer mental wellness. Suicidal ideation is notwithstanding some other major business organisation for adolescents during the pandemic. While suicide was the 10th leading cause of deaths overall in the U.S. before the pandemic, information technology was the 2d leading crusade of deaths amongst adolescents ages 12 to 17.viii Prior to the pandemic, suicide rates were particularly pronounced among Black and LGBTQ youth.
Communities of Color
The pandemic's mental health impact has been pronounced amidst the communities of color too experiencing disproportionately high rates of COVID-xix cases and deaths. Black and Hispanic adults take been more likely than White adults to report symptoms of anxiety and/or depressive disorder during the pandemic (Figure 7). This disparate mental health affect comes in improver to Black and Hispanic communities experiencing disproportionately high rates of coronavirus cases and deaths (overall as well equally among health care workers and in nursing homes), and negative financial impacts. Additionally, Blackness parents more than often than White parents have reported negative impacts of the pandemic on their children's education, their ability to intendance for their children, and their relationships with family members. Prior to the pandemic, Blackness and Hispanic people were less likely to receive needed behavioral wellness services compared to the general population. Additionally, deaths by suicide – which may increase due to the pandemic – have historically been much higher than average amongst Native American communities.
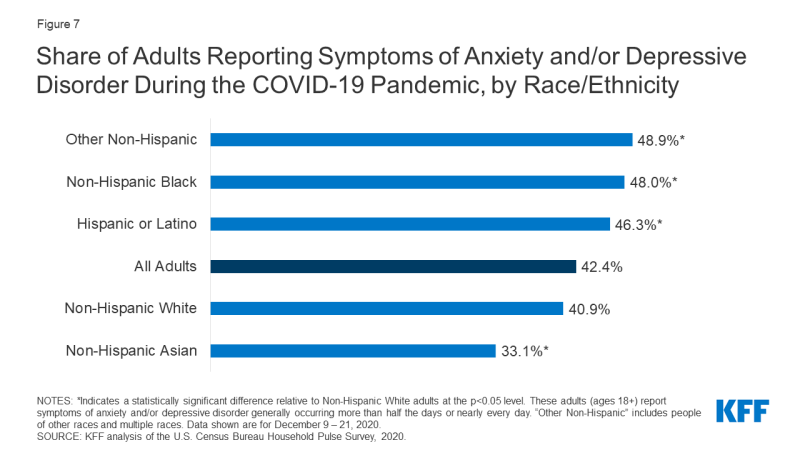
Figure vii: Share of Adults Reporting Symptoms of Anxiety and/or Depressive Disorder During the COVID-19 Pandemic, by Race/Ethnicity
Essential Workers
Essential workers during the COVID-xix pandemic, such equally health care providers, grocery store employees, and post and package delivery personnel, take shown loftier rates of poor mental health outcomes. These workers are generally required to work outside of their home and may be unable to practise social distancing. Consequently, they are at increased take chances of contracting coronavirus and exposing other members of their household. A KFF analysis found that essential workers confront additional challenges, including difficulties affording basic necessities every bit a result of the pandemic. These factors may contribute to poor mental health outcomes for these workers. Every bit shown in Figure eight, essential workers are more probable than nonessential workers to report symptoms of anxiety or depressive disorder (42% vs. 30%, respectively), starting or increasing substance use (25% vs. 11%), or considering suicide in the past 30 days (22% vs. viii%).
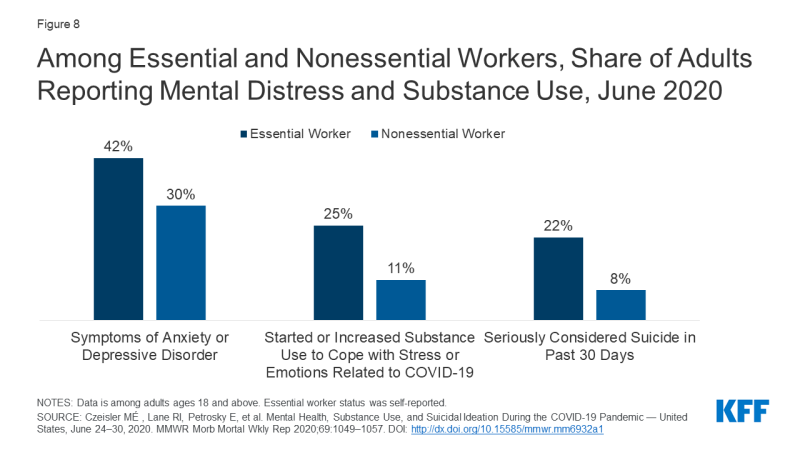
Figure 8: Amid Essential and Nonessential Workers, Share of Adults Reporting Mental Distress and Substance Use, June 2020
During the pandemic, frontline health care workers take reported feelings of anxiety and depression and thoughts of suicide. The KFF Health Tracking Poll conducted in mid-April 2020 found that 64% of households with a wellness intendance worker said worry and stress over the coronavirus acquired them to experience at least one adverse affect on their mental health and well-being, such as difficulty sleeping or eating, increases in alcohol consumption or substance use, and worsening chronic conditions, compared to 56% of all households. Prior to the pandemic, nurses and physicians were already prone to experiencing burnout, with physicians also having an elevated take chances of suicide.
Policy Responses and Considerations
Throughout the pandemic, leading public health organizations — including the CDC, SAMHSA, the World Health Arrangement, and the United nations — take released general considerations and resources addressing the mental health and well-existence of both general populations and specific, high-take a chance groups during the pandemic. In the U.Southward., some steps have been taken at both the federal and state levels to address the pandemic'south touch on mental health, but with mental health issues on the rising, primal issues are probable to persist.
Congress has addressed some of the acute need for mental health and substance use services through two stimulus bills enacted during the pandemic. The Consolidated Appropriations Human activity, which was signed into law in December 2020, includes nearly $four.25 billion in funding for mental health and substance use services. Information technology also builds on existing legislative efforts to boost insurer compliance with federal mental health parity rules. The Coronavirus Aid, Relief, and Economic Security Act (CARES Act), a stimulus bill passed in March 2020, also allocated funding for mental health and substance use services, including a $425 million appropriation for utilize by SAMHSA, in addition to several provisions aimed at expanding coverage for, and availability of, telehealth and other remote care for those covered by Medicare, private insurance, and other federally-funded programs. It also allowed for the Section of Veterans Affairs to arrange expansion of mental wellness services to isolated veterans via telehealth or other remote care services. Other efforts to address mental wellness needs include substantial increases in the use of telehealth for mental health services, aided early by the federal government and many states expanding coverage and relaxing regulations for telehealth services. Looking ahead, the Biden administration and Congress could accept additional steps to address mental health and substance apply issues, including authoritative actions addressing suicide amongst LGBTQ youth, mental health parity, the opioid crunch, veteran mental wellness services, and school-based mental health services.
Given the pandemic'due south implications for both people with new or pre-pandemic mental health conditions, the crisis spotlights new and existing barriers to accessing mental health and substance use disorder services. Amongst adults reporting symptoms of anxiety and/or depressive disorder, more than 20% report needing but non receiving counseling or therapy in the past month during the pandemic. Limited admission to mental health care and substance use treatment is in part due to a current shortage of mental health professionals, which has been exacerbated by the pandemic. The pre-pandemic shortage of psychiatric hospital beds has also worsened with the surge of COVID-nineteen patients needing beds at hospitals across the nation.
Access to mental health and substance use care was a concern prior to the pandemic. In 2018, among the 6.5 one thousand thousand nonelderly adults experiencing serious psychological distress, 44% reported seeing a mental wellness professional in the past year. Compared to adults without serious psychological distress, adults with serious psychological distress were more likely to exist uninsured (20% vs 13%) and be unable to afford mental health intendance or counseling (21% vs 3%).9 For people with insurance coverage, an increasingly common barrier to accessing mental wellness care is a lack of in-network options for mental health and substance utilize care. Those who are uninsured already face paying full price for these and other wellness services. As unemployment continues to affect millions of people, who in turn may lose job-based coverage, some may regain coverage through options such every bit Medicaid, COBRA, or the ACA Marketplace, but others may remain uninsured. With an unprecedented share of people reporting symptoms of feet or depressive disorder, the potential outcome of California five. Texas (a case challenging the constitutionality of the entire ACA) is of import to consider. Prior to the ACA, people with a preexisting condition like depression might have been denied wellness coverage or charged higher premiums, and many individual market plans did not cover any mental health or substance employ services.
Looking Ahead
The pandemic has both short- and long-term implications for mental wellness and substance use, peculiarly for groups at risk of new or exacerbated mental health disorders and those facing barriers to accessing intendance. Phased COVID-nineteen vaccinations are taking identify across the country, perhaps signaling that the end of the pandemic is on the horizon. However, many of the stressful weather employed to mitigate the spread of the coronavirus are probable to persist for the near futurity, given the slow and troubled rollout of vaccinations across the country, instances of people refusing the vaccine due to fear or doubtfulness, and the need for vaccinated people to continue taking existing precautions to mitigate the outbreak.
History has shown that the mental health impact of disasters outlasts the concrete impact, suggesting today's elevated mental health demand will proceed well beyond the coronavirus outbreak itself. For case, an analysis of the psychological toll on health care providers during outbreaks found that psychological distress tin can final up to 3 years after an outbreak. Due to the fiscal crisis accompanying the pandemic, at that place are as well pregnant implications for mortality due to "deaths of despair." A May 2020 assay projects that, based on the economic downturn and social isolation, additional deaths due to suicide and alcohol or drug misuse may occur by 2029.
As policymakers keep to discuss further actions to alleviate the burdens of the COVID-19 pandemic, it will exist important to consider how the increased need for mental health and substance use services volition likely persist long term, even if new cases and deaths due to the novel coronavirus subside.
This piece of work was supported in function by Well Being Trust. Nosotros value our funders. KFF maintains full editorial command over all of its policy analysis, polling, and journalism activities.
urbinafesionfluen.blogspot.com
Source: https://www.kff.org/coronavirus-covid-19/issue-brief/the-implications-of-covid-19-for-mental-health-and-substance-use/
Postar um comentário for "Impact of Mental Illness on Individuals and Families"